By Kirsten Steinman
EDITOR’S SUMMARY: Quiet but powerful, vitamin K shapes the body’s most essential systems—from the first days of life to the final decades. How it’s understood, delivered, and nourished over time can influence not only immediate health but the foundation for resilience across a lifetime. Found abundantly in leafy greens, organ meats, cheeses, and fermented foods, it’s both a nutrient of nature and a pharmaceutical intervention. In newborn care, the ongoing debate between injectable and oral forms highlights the tension between public health policy and personal choice.
You want to age well—to move freely, think clearly, and live long enough to truly enjoy life. Some of your body’s most critical structures and organs—bones, heart, brain, and even blood vessels—determine not just how long you live but the quality of your life. Heart disease remains the leading cause of death worldwide, while weak, fracture-prone bones can silently steal independence in later years. Meanwhile, stiff arteries and cognitive decline often go unnoticed, eroding vitality long before old age sets in.
What’s less well known than the conditions themselves is how tightly these key players are linked: stronger bones protect the heart, and healthier blood vessels and brain function depend on the same nutrients that fortify the skeleton. The nutrient at the center of that connection? Vitamin K. Once thought of only as a clotting factor—a substance that helps stop excessive bleeding by forming a fibrin mesh to seal a wound—it’s now emerging as one of the body’s most underappreciated defenders of health and vitality, critical for keeping bones strong, arteries flexible, and your mind sharp from youth to old age.
You may have grown up believing bone health started with a glass of milk at the table. Thanks to the iconic “Got Milk” ads of the 90s, calcium became synonymous with strong bones. But calcium is only one part of the equation. Without the right supporting cast—nutrients like vitamin C, D, and especially vitamin K—calcium can end up in all the wrong places, such as soft tissue and arteries. When it settles in blood vessels, it can cause them to stiffen, increasing your risk of heart damage or heart attack. In muscles and connective tissue, these deposits may lead to inflammation and pain. The result: you might meet your daily calcium requirements and still be setting yourself up for brittle bones or clogged arteries if vitamin K is lacking.
Vitamin K first emerged in 1934, when Danish scientist Carl Peter Henrik Dam discovered its role in blood clotting. For decades, that was its claim to fame. But by the 1970s, research revealed a much broader influence—one that extends well beyond coagulation. Clinical trials have shown that high doses of vitamin K can increase bone mineral density and reduce fracture risk in people with osteoporosis. It does this by activating proteins like osteocalcin, essential for bone formation, and matrix GLA protein (MGP), which prevents calcium from hardening the arteries. MGP is especially powerful: beyond supporting bone health, it regulates clotting by producing four key coagulation factors—II (prothrombin), VII, IX, and X. Without them, serious conditions like stroke, deep vein thrombosis, or heart attack can occur.
K1 and K2: A Tale of Two Pathways
There are two types of vitamin K: vitamin K1 (phylloquinone) is primarily found in leafy green vegetables such as spinach, broccoli, kale, and Swiss chard. It supports clotting but doesn’t circulate well beyond the liver, which is why K2 plays a bigger role in bone, heart, and brain health. Vitamin K2 (menaquinone) is found in various sources, including fermented foods (miso, sauerkraut, natto) and animal foods (eggs, hard cheeses, beef liver). Among the K2 family (known as MKs), MK-4 is unique—it’s not produced microbially but occurs naturally in animal foods. MK-7 through MK-13, on the other hand, are made by microbes and concentrated in fermented foods. Not all sources are created equal—grass-fed organ meats and dairy fat, for example, contain higher amounts of K2 because cows convert the K1 in grass into K2 in their tissues. Lean cuts like steak or ground beef also reflect this conversion, but in lower concentrations.
K1 is easy to get if your diet includes vegetables, but K2 is the form more often used in supplements—especially when the focus is on bone, heart, or brain health. Most vitamin K supplements are synthetic, meaning they’re made in a lab rather than extracted directly from foods. K1 and MK-4 are almost always produced this way, though they’re bioidentical—chemically the same as what your body would get from natural sources. MK-7, on the other hand, is often made through bacterial fermentation of soybeans, which are commonly genetically modified unless labeled otherwise. Choosing products made from non-GMO or organic soy can help ensure higher quality and align with personal dietary preferences. Your body can also make its own K2, thanks to beneficial gut flora, which may supply over half of your daily needs. A high-fiber diet supports K2-producing species like Lactobacillus and Bifidobacterium.
While vitamins K1 and K2 share a core structure, they behave differently in the body. The longer side chains of K2 act like anchors, allowing it to travel from the liver into the bloodstream and linger for days—protecting bones and arteries. K1, with its much shorter half-life, stays in the liver for just hours and focuses mainly on clotting.
The Framingham Heart Study—an ongoing observational project—found that vitamin K1 intake was linked to lower inflammation and fewer broken hips in older adults. An extensive review of multiple long-term trials, “Vitamin K status, cardiovascular disease, and all-cause mortality: a participant-level meta-analysis of 3 US cohorts,” confirmed that low circulating levels of K1 are associated with higher all-cause mortality. People at risk of vitamin K deficiency (both K1 and K2) include those with chronic conditions such as non-alcoholic fatty liver disease and chronic kidney disease, as well as individuals with severe malnutrition, absorption issues, heavy alcohol consumption, or long-term antibiotic use.
Emerging research points to vitamin K’s role in brain health. In animal studies, vitamin K2 deficiency increased inflammation in the hippocampus—the brain’s memory center—leading to impaired learning and recall. Deficient mice struggled with tasks that tested object recognition and spatial memory, while those with adequate vitamin K2 performed significantly better. These findings suggest that vitamin K’s influence may extend to protecting against cognitive decline and neurodegenerative disease. As noted by Tufts University in “New Research Deepens Understanding of How Vitamin K Affects Brain Health,” the evidence continues to build:
“In one such test, the novel object recognition test, the vitamin K-deficient mice showed a diminished ability to distinguish between familiar and new objects, a clear indication of impaired memory. In a second test, to measure spatial learning, the mice were tasked with learning the location of a hidden platform in a pool of water. The vitamin K-deficient mice took considerably longer to learn the task compared to their counterparts with adequate vitamin K levels.”
Like most nutrients, vitamin K doesn’t work alone. Its partnership with vitamin D—specifically K2 and D3—is essential for calcium balance. Vitamin D enhances calcium absorption in the intestines, while vitamin K directs the calcium to the bones and teeth and away from arteries. This nutrient synergy has long roots: in the 1930s, Dr. Weston A. Price, a pioneering dentist and researcher, observed that traditional diets rich in fat-soluble compounds seemed to protect against tooth decay and skeletal deformities.
Through experiments in both animals and humans, he identified a mysterious “Activator X,” now recognized as vitamin K2 (specifically MK-4). In one of his studies, rats given “butter vitamins” (his term for concentrated K2) developed stronger bones and joints—especially when paired with cod liver oil, a natural source of vitamins A and D. Price’s findings anticipated what modern science now confirms: vitamins A and D signal the body to produce bone-building proteins, and vitamin K2 activates them—an elegant interplay that keeps calcium where it belongs. From the Weston A. Price Foundation article “Vitamin K2 MK-4: Dr. Price’s Activator X and Its Transformational Potential”:
“In short, the problems Price witnessed in his practice came from nutritionally deficient diets. He proved that when modern foods replaced traditional diets full of fat-soluble ‘activators’ (vitamins), dental disease and physical degeneration occurred. Surprisingly, this knowledge remains lost or hidden in our modern society. Has your dentist ever told you that you needed to get more grass-fed animal fat in your diet or that you needed more vitamin K2 MK-4?”
Sunlight is the best source of vitamin D3: exposing arms and legs for 10 to 60 minutes a day—depending on skin tone, season, and latitude—allows your body to produce what it needs naturally. Balance is key—getting too much vitamin D from supplements without enough vitamins K1 and K2 can disrupt calcium regulation, underscoring the importance of natural sources and mindful supplementation.
Beyond bones, heart, and brain, emerging evidence hints at another surprising benefit—potential anti-cancer effects. Vitamin K2 has been shown to slow tumor growth by prompting cancer cells to halt their cycle and self-destruct. In Japan, a 2023 investigation, “Vitamin K Intake and Risk of Lung Cancer: The Japan Collaborative Cohort Study,” found that higher dietary vitamin K intake was associated with lower lung cancer risk, particularly in men and current smokers (the authors noted they could not separate intakes of K1 and K2). Earlier, a 2004 JAMA study, “Role of Vitamin K2 in the Development of Hepatocellular Carcinoma in Women With Viral Cirrhosis of the Liver,” showed women with viral liver disease who took vitamin K2 were significantly less likely to develop hepatocellular carcinoma. Laboratory experiments support these findings, demonstrating K2’s potential in liver, bile duct, ovarian, pancreatic, colorectal, and certain blood cancers.
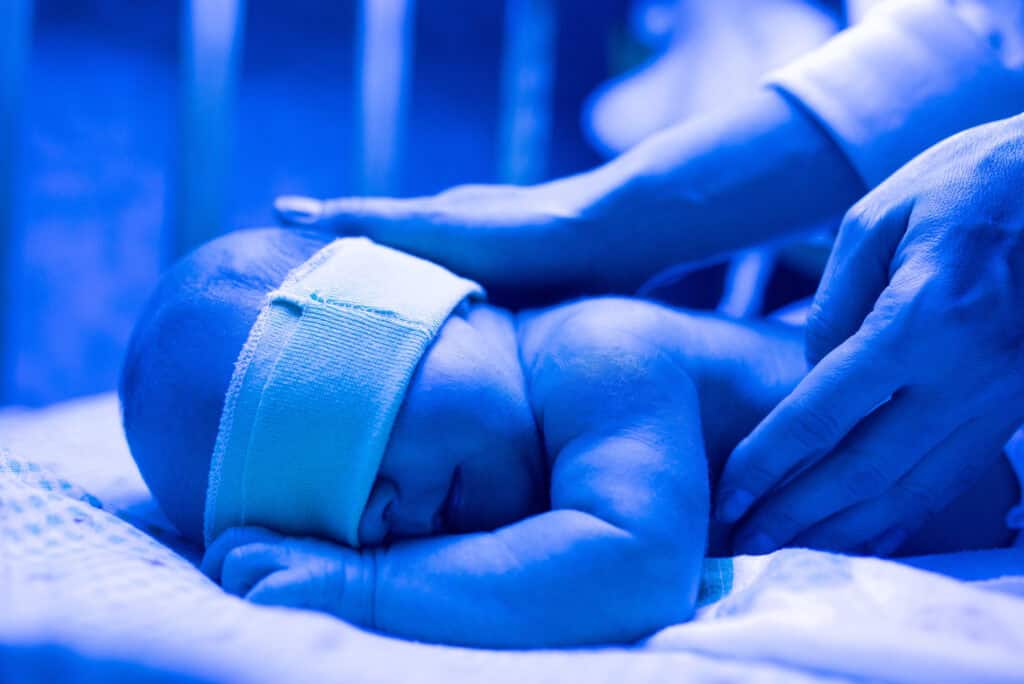
Vitamin K at the Very Beginning
For adults, vitamin K is a clear ally for healthy aging. But in newborns, its role is more complex. Babies are born with low vitamin K: little crosses the placenta, their sterile guts can’t yet produce it, and breastmilk contains only trace amounts (1–9 mcg/L, compared with up to 57 mcg/L in most infant formulas). This has long been labeled a “deficiency” and used to justify supplementation at birth. In the United States, supplementation began in the 1940s with oral vitamin K3 (menadione), but this was abandoned after it was linked to cases of jaundice—yellowing of the skin and eyes caused by excess bilirubin—and hemolytic anemia, a condition in which red blood cells break down faster than the body can replace them. When bilirubin levels run high, babies are typically treated with blue light phototherapy—a safe, noninvasive intervention that helps a newborn’s body break down bilirubin for excretion. By the 1970s, the standard shifted to injectable synthetic K1 (phytonadione)—still the only FDA-approved option today. Both the oral and injectable forms are intended to prevent vitamin K deficiency bleeding (VKDB), which comes in three forms:
- Early VKDB: Rare and usually associated with maternal medications that interfere with vitamin K metabolism, such as certain anticonvulsants or tuberculosis drugs. These medications can cross the placenta and suppress the newborn’s ability to activate clotting factors, setting the stage for bleeding episodes within the first 24 hours of life.
- Classic VKDB: Appears 2–7 days after birth, often tied to traumatic delivery (such as forceps or vacuum extraction), delayed feeding, or premature cord clamping. Premature clamping of the umbilical cord can deprive babies of up to 40% of their natural blood volume—including clotting factors and platelets.
- Late VKDB: Typically appears between 8 days and 6 months of age, most often in exclusively breast-fed infants, and can present as dangerous intracranial bleeding. According to the American Liver Foundation, during the first month after birth the incidence of neonatal liver disease is as high as one in 2,500.
Supplementation is aimed primarily at preventing late VKDB, which can strike suddenly without warning and carries a higher risk of life-threatening complications. While prevention is a worthy goal, the current approach overlooks another reality: too much vitamin K in infants can also be harmful. Toxicity—though not widely reported—has been linked to ruptured blood cells, severe jaundice, and kernicterus, a rare type of brain damage. These effects have been documented primarily following vitamin K1 injections, particularly in premature newborns.
Beyond the nutrient itself, the injectable solution may include excipients such as polysorbate 80, propylene glycol, benzyl alcohol, dextrose, sodium acetate, aluminum, and sometimes hydrochloric acid (depending on the manufacturer/formulation). The Pfizer product insert contains a black box warning about severe, sometimes fatal, reactions. It advises against intravenous or intramuscular use unless subcutaneous administration (into the layer of fat just below the skin) is not possible and “the serious risk is justified.” Yet despite this caution, the American Academy of Pediatrics continues to recommend that all newborns receive the shot directly into muscle tissue. Premature infants are especially vulnerable. As the March of Dimes explains:
“Babies born preterm- before 37 weeks of pregnancy—are more likely than full-term babies to develop jaundice because their livers aren’t fully developed or functional yet. It can take a week or more for a preterm baby’s liver to become fully functional.”
Aluminum, a component of the injection, is primarily filtered by the kidneys, and delayed excretion allows it to accumulate in the body. This can lead to multi-system toxicity, most notably affecting the brain and bones. Recognizing this, the FDA requires a warning on the product label advising against use in premature infants. In recent years, the dosage has been lowered for babies born before 37 weeks—but aluminum remains in the injection.
Benzyl alcohol, another additive, has been linked to “gasping syndrome,” a fatal condition first identified in premature infants in the 1980s. Accumulation in the body can trigger symptoms including gasping respiration, central nervous system depression, intracranial hemorrhage, cardiovascular collapse, kidney and liver failure, and seizures. The FDA issued a safety advisory in 1982 warning against intramuscular solutions containing benzyl alcohol after reports of neonatal deaths—defined as occurring within the first 28 days of life. Studies have shown that this preservative can damage the membranes of cells lining the digestive tract, further highlighting the vulnerability of newborns to additives in the injection.
In the U.S., the prevailing view is that oral vitamin K is less effective than the injectable form at treating deficiency in newborns because of concerns about vomiting, poor absorption, or parents not completing the regimen. Globally, however, many countries take a different approach. The Netherlands, France, Switzerland, and Japan all recommend oral supplementation at birth. In Switzerland, newborns receive two oral doses (at birth and on day four), and their late VKDB rate is less than 0.87 per 100,000 births. In the United States, rates are higher—around 3.2 per 100,000 among infants who receive the injection, and 4.4–7.2 per 100,000 among those who receive no vitamin K.
A 2025 analysis in JAMA examining more than 5 million U.S. births from 2017–2024 found that the number of newborns not receiving intramuscular vitamin K has nearly doubled—from just under 3% to just over 5%. Nonreceipt was most common among vaginal births and non-Hispanic white families. Rather than exploring the reasons behind this rise in parental hesitancy, the authors characterized it as a public health problem and recommended “multipronged” efforts to increase injection uptake, including standardized clinician messaging and potential state-level regulatory strategies.
Supporting oral supplementation, a 1997 clinical study in the Philippines tested a multi-dose regimen of vitamin K2 (synthetic MK-4) in eighty healthy, full-term breastfed infants. Researchers compared the results of oral K2 supplementation to those from the standard single-dose K1 injection and, to their surprise, found that oral K2 was comparable in efficacy to the injectable K1. Together, these findings suggest that oral vitamin K—especially in the K2 form—may offer a viable and effective alternative to injections when administered correctly and consistently.
Another unexplored option is maternal supplementation. A 1997 trial by Greer et al. in the American Academy of Pediatrics, “Improving the Vitamin K Status of Breastfeeding Infants With Maternal Vitamin K Supplements,” found that giving mothers a daily dose of 5 mg of vitamin K1 boosted breast milk concentrations to levels that could meaningfully raise infant intake. More recently, a 2022 review in Pediatrics, “Vitamin K and the Newborn Infant,” reaffirmed maternal supplementation as a strategy that can enhance vitamin K levels in breastfed infants, though it’s not widely implemented in the U.S. By the end of the first week of life, most breastfed babies are also producing some of their own vitamin K, thanks to colonization of the gut during birth and breastfeeding.
Passage through the birth canal exposes infants to maternal microbes (babies often face the rectum, which is no accident), while colostrum—the nutrient-dense early milk—is rich in prebiotics and probiotics, including Lactobacillus and Bifidobacterium, which help establish a healthy microbiome. That microbiome, however, is fragile. While some factors strengthen microbial diversity and vitamin K2 production, others can disrupt it. Antibiotics, for example, are a major disruptor—wiping out beneficial bacteria, reducing diversity, and allowing opportunistic strains to dominate. An imbalanced gut makes it harder for infants to produce vitamin K2 effectively.
Newborns being “deficient” in vitamin K is not new—it has been true throughout human history. This raises an important question: did nature really make a mistake, or is low vitamin K only a problem in the context of interventions like infant circumcision and forceps delivery, both of which increase bleeding risks? In 1893, physician Jacobsen published one of the earliest medical warnings on bleeding risk in newborns, urging clinicians to assess familial bleeding tendencies before circumcision. He cited four related cases in which all infants died from hemorrhage following the procedure. Decades later, even with the adoption of the clamp method, misplacement or improper technique could still trigger dangerous bleeding.
Modern research adds another layer: a 2018 NIH study, “Intracranial bleeding due to vitamin K deficiency: advantages of using a pediatric intensive care registry,” examining 16 infants with late VKDB found that 75% were male—suggesting that biological sex may increase vulnerability beyond medical interventions. A 2021 survey published in the Journal of Pediatric Urology echoed this complexity, with nearly one-third of respondents noting that hyperbilirubinemia—the liver’s reduced ability to process bilirubin—can make circumcision particularly risky. Together, historical and contemporary data underscore that males face a higher danger of late VKDB, particularly when combined with procedures like circumcision or premature cord clamping.

A Nutrient That Spans a Lifetime
For adults, vitamins K1 and K2 may be some of the most underrated nutrients for aging well—fortifying your bones, protecting your heart and other vital organs, and supporting your brain. For infants, the story is more nuanced, shaped not only by biology but by modern intervention. In the U.S., the injectable form of vitamin K1—while effective at protecting against deficiency—has raised concern due to the additional ingredients it contains, prompting some parents to explore oral vitamin K2 alternatives used safely in other countries.
What’s clear across your lifespan is that vitamin K is far from a minor player and instead acts as a silent steward—guiding calcium, supporting critical systems, and maintaining balance throughout your body. It deserves careful thought—from the foods you eat to the policies that shape your choices at birth. As science continues to unfold the mysteries of vitamin K, your willingness to question assumptions, weigh risks and benefits, and make informed choices must evolve too. Whether your goal is to age strong or give a newborn the best start, understanding vitamin K is one of the most powerful steps you can take toward lifelong health. Start today—fill your plate with leafy greens for K1 and add organ meats, cheese, dark chocolate (80% cacao or higher) and fermented foods for K2. Support your gut health with fiber and probiotics, get adequate vitamin D from sunlight, and talk to a trusted integrative provider or certified midwife about oral vitamin K options for your baby.
If you choose to supplement, quality matters. Look for whole-food fermented sources like organic natto or non-soy fermentation (such as chickpeas) rather than purely synthetic ingredients. MK-7 derived from fermentation is often better absorbed and has a longer half-life in the body than synthetic MK-4. Third-party testing, no additives, and transparent ingredient sourcing can help ensure a cleaner product. If MK-4 is your preference, choose bioidentical forms without fillers or preservatives. Small, intentional choices like these can fortify your health at its foundation, laying the groundwork for strength and resilience that lasts for decades.
~
Published on December 11, 2025.
If you’ve found value in this article, please share it!
To support the research and health education of AVFC editorial, please consider making a donation today. Thank you.


